Diabetic Eye Disease Evaluation and Treatment
Diabetes can create several problems for the eyes, including fluctuations with eyeglasses prescriptions, cataracts at a younger age, and increased risk to develop glaucoma. However, the most serious complication is diabetic retinopathy. The retina is the wall paper-like structure which lines the back of the eye. It is responsible for turning light into vision, and is nourished by numerous blood vessels. With diabetes, the normal retinal blood vessels can begin to leak blood, fluid, and cholesterol/lipid deposits onto the retina (backround diabetic retinopathy). In addition, abnormal blood vessels can form (proliferative diabetic retinopathy). These abnormal blood vessels can cause tremendous bleeding and scarring of the retina.
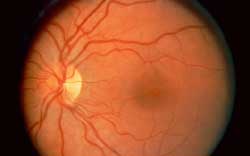
Normal retina. The optic nerve is the round yellow structure. Exiting out of the optic nerve are the normal blood vessels of the retina.
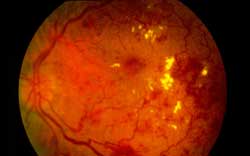
Backround diabetic retinopathy. There is leakage of blood (dark red blotches) and cholesterol/lipids (yellow deposits) onto the retina.
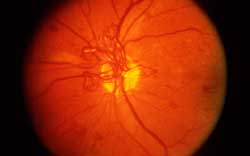
Proliferative diabetic retinopathy. There are numerous small, tortuous, abnormal blood vessels.
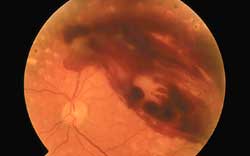
Proliferative diabetic retinopathy. There is a large hemorrhage arising from the abnormal blood vessels.
The longer a person suffers from diabetes, the greater the likelihood of developing diabetic retinopathy. After 5 years of diabetes, there is a 20% likelihood of developing retinopathy, and after 15 years, there is an 80% likelihood. Diabetic retinopathy is the leading cause of blindness in all persons between 20 and 64 years old in the United States.
Proper blood sugar control is the best way to lower the likelihood of developing diabetic retinopathy. However, even with seemingly excellent control, the process may still occur. Therefore, all diabetics should have their eyes examined at least once a year and more often if problems develop. Early detection and management are critical because many of the blinding complications are treatable and preventable, but once damage has occurred it is often permanent.
The primary treatment for diabetic retinopathy is laser therapy. Laser treatment is recommended if the leakage of blood, fluid, or cholesterol is near the macula (the center of the retina, the area responsible for central vision). In these cases, laser burns are directed to “seal up” the areas of leakage. Laser therapy is also recommended if abnormal blood vessels form. In these cases, the laser burns are directed all over the peripheral retina. The effect of these burns is to cut off the stimulus for the abnormal blood vessels to grow, and indirectly cause them to shrink away and regress. In severe cases, incisional surgery may be required to remove blood and/or scar tissue (vitrectomy surgery).
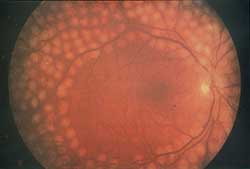
Hundreds of laser burns were placed to cause the abnormal blood vessels to shrink away.
For more information about diabetic retinopathy, go to: www.nei.nih.gov/health/diabetic/retinopathy.htm.